Story Highlights:
- THC can increase heart rate by 20-50 beats per minute. This increase occurs in order to compensate for the reduction in blood pressure caused by THC.
- Low doses of THC appear to most strongly activate pro-cardiovascular health effects. At higher THC doses, the effect on CB1 receptors overrides THC’s effect on CB2 receptors and has a net negative impact on cardiovascular health.
- CBD has beneficial effects on cardiovascular risk factors and improves recovery in animal models of heart attack and stroke. Consumers with heart concerns should gravitate toward high-CBD/low-THC strains.
- Cardiovascular events only represent 2% of all medical reports related to cannabis.
- Synthetic cannabinoids like “K2” and “Spice” pose the greatest risk of heart and health complications, and should be avoided by all consumers.
There are over 630,000 deaths annually in the United States due to heart disease, which represent nearly a quarter of all deaths. An additional 140,000 deaths result from stroke. Cannabis consumers are used to warnings about the potential damage the drug is doing to their brain, but what about their heart? Could cannabis be affecting our cardiovascular health?
The cardiovascular system is made up of the heart and blood vessels that transport blood throughout your body (the “cardio” part of the term refers to the heart, while “vascular” refers to the system of blood vessels, veins, and arteries). When the cardiovascular system isn’t working properly, it can lead to a heart attack, where part of the heart muscle dies, or a stroke, which is the blockage or rupture of blood vessels that then deprives brain cells of their necessary nutrients and causes them to die.
In a recent meta-analysis, researchers scrutinized 24 articles that investigated the impacts of cannabis on cardiovascular risk factors (such as cholesterol levels, obesity rates, and diabetes) and cardiovascular events like stroke and heart attack. They concluded that there’s insufficient evidence that cannabis use has any effect on heart attacks or stroke, or increases their risk factors. In fact, the researchers found some evidence that cannabis use may be associated with lower risk for obesity.
So are cannabis consumers in the clear? Not so fast. The authors note that many of the studies were limited by elevated risk of bias and poor control over cannabis exposure levels and frequency. Also, because levels of the euphoric cannabinoid THC are on the rise, it’s difficult to generalize the effects of cannabis use over the last few decades using today’s use patterns.
But what caused scientists and physicians to propose a link between cannabis and cardiovascular risk factors in the first place?
Increase in Cannabis-Related Health Complications in the Clinic
With the number of cannabis consumers increasing, so have the number of cannabis-related cardiovascular events. The problem is that the cannabis consumers showing up in emergency rooms are often young with few other risk factors, leading many to believe that cannabis itself is playing a role.
Most studies looking at the impact of cannabis on cardiovascular health only control for general use patterns, not type of cannabis.
One study found that risk of heart attack increases nearly five-fold within the hour of using cannabis. Another found that weekly cannabis use more than quadruples stroke risk. You’d predict then, that if cannabis access increases with legalization, cardiovascular deaths would go up. Indeed they do, and the effect is strongest in states with more lax dispensing regulations.
Well, that sounds frightening. If it’s true, how could another study conclude that there’s no sufficient evidence for cannabis’ effect on cardiovascular complications?
Variability in Cannabis Type and Use Patterns Makes Studies in Humans Challenging
Your average dispensary has a massive range of cannabis products available. Some are rich in THC, while others are low in THC. Some have high levels of other cannabinoids, like cannabidiol (CBD), which can have opposite effects on the brain and body as THC. But most studies looking at the impact of cannabis on cardiovascular health only control for general use patterns, not type of cannabis.
The studies usually don’t control for THC consumption or the presence of other cannabinoids. The larger assessments of the impact of statewide legalization on cardiovascular events in the state’s population don’t even assess whether these events occurred in cannabis users, thereby assuming that increased cannabis access is the variable that changed the mortality rate. So when someone says that “cannabis use” increases risk for cardiovascular events, the next questions should be “what type of cannabis? And how often are they using?”
To better understand the impact of cannabis on the heart and vasculature, let’s unpack the contribution that the endogenous cannabinoid receptors type I and II (CB1 and CB2) have on cardiovascular function.
The Impact of CB1 Receptors on Heart Rate and Heart Attack Risk

THC activates CB1 receptors to decrease blood pressure and increase heart rate. (Elysse Feigenblatt/Leafly)
CB1 receptors are found all over the body’s cardiovascular system. They’re on the heart muscle, surround blood vessels, and regulate the brain nerves that control heart rate. So there’s plenty of reason to believe THC-rich cannabis could impact cardiovascular function.
Increased Heart Rate
Activation of CB1 receptors by THC can increase heart rate by 20-50 beats per minute. This increase occurs in order to compensate for the reduction in blood pressure caused by THC. Blood pressure is lowered because THC increases the diameter of blood vessels, forcing the heart to work harder in order to pump blood. Some reports find that the heart must work 30% harder in the presence of high levels of THC.
Effects on Arteries
CB1 receptor activation also increases plaque buildup in arteries, which increases risk of atherosclerosis, a disease characterized by the narrowing of arteries that can lead to heart attack and stroke. This effect occurs through two main mechanisms.
First, activating CB1 receptors increases the amount of harmful chemicals called reactive oxygen species, which damage the walls of arteries. The damage to the artery walls initiates an immune response that attracts special immune cells known as macrophages. These macrophages become part of the wall of the artery.
This is worsened by a second effect of activating CB1 receptors, which increases the amount of the “bad” low-density lipoprotein (LDL) cholesterol of the macrophages that adhere to the walls of the artery. Elevated levels of reactive oxygen species have an exacerbated effect on plaque buildup, increasing risk of heart attack and stroke.
The Effects of CB2 Receptors on Cardiovascular Health
While drugs that activate CB1 receptors can have negative effects on cardiovascular health, drugs that selectively activate CB2 receptors have beneficial effects on heart health.
Low doses of THC have been shown to reduce plaque buildup and risk for atherosclerosis.
CB2 receptors are mostly expressed in immune cells, but their levels increase in other parts of the body after injury or in disease. Therefore, they’re not only a good target to reduce the harmful effects of CB1 receptors on heart health, they can be a promising target to lessen the damage caused by injury or cardiovascular attack.
Activating CB2 receptors reduces the inflammation and free radicals that increase plaque buildup in arteries and elevate risk for heart attack and stroke. Through this anti-inflammatory effect, if a heart attack or stroke does occur, activating CB2 receptors reduces the extent of damage.
Shop highly rated dispensaries near you
Showing you dispensaries nearIs THC Dangerous for Cardiovascular Health?
The answer depends on the dose. THC can activate both CB1 and CB2 receptors, but low doses of THC appear to most strongly activate CB2’s pro-cardiovascular health effects. At higher doses, THC’s effect on CB1 receptors overrides its effect on CB2 receptors and has a net negative impact on cardiovascular health.
In fact, low doses of THC have been shown to reduce plaque buildup and risk for atherosclerosis. This beneficial low-dose effect is thought to come from THC’s activation of CB2 receptors and not CB1 receptors, suggesting that THC’s ability to activate CB2 receptors can protect the heart, while its activation of CB1 receptors can hurt it.
How Other Cannabinoids Affect Cardiovascular Health
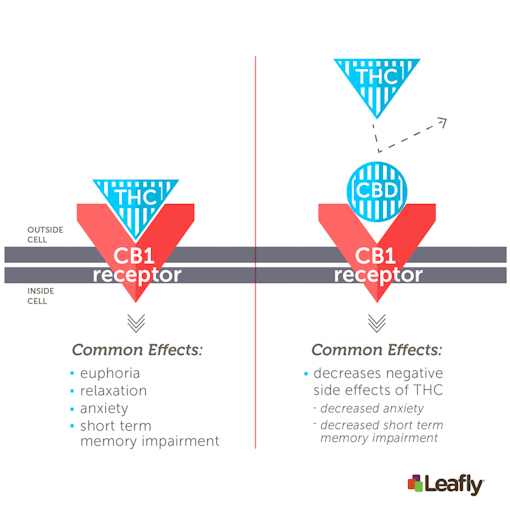
Left: THC directly stimulates the CB1 receptor. This interaction underlies the major psychoactive effects of cannabis consumption. Right: CBD reduces, or “antagonizes,” THC’s ability to stimulate CB1 receptors. (Amy Phung/Leafly)
Two of the most abundant phytocannabinoids other than THC are CBD and tetrahydrocannabivarin (THCV). CBD can block THC’s ability to activate CB1 receptors and could protect against some of the harm caused by the drop in blood pressure and elevated heart rate caused by THC alone.
On its own, CBD is a potent antioxidant and neutralizes harmful free radicals. It also has strong anti-inflammatory abilities which can reduce the damage caused by activation of CB1 receptors. Indeed, CBD has beneficial effects on cardiovascular risk factors and improves recovery in animal models of heart attack and stroke.
THCV has pro-cardiovascular effects by blocking CB1 receptor function at low doses. It’s through this mechanism that THCV is thought to reduce insulin sensitivity in obese mice, which reduces risk for cardiovascular events. And like CBD, THCV has been shown to be safe in Phase II clinical trials. THCV becomes an activator of CB1 receptors at high does, but in most strains of cannabis, THCV levels are too low to activate them.
Find CBD Cannabis Strains
Synthetic Cannabinoids Can Cause Death
Synthetic cannabinoids, particularly those that try to mimic THC, have been linked with numerous severe health consequences. Given the impact that activating CB1 receptors can have on cardiovascular health, this shouldn’t be surprising.
For instance, synthetic cannabinoids like “K2” and “Spice” are 2-100 times better at activating CB1 receptors than THC. Even after a single use, synthetic cannabinoids have been linked with numerous cases of medical emergencies involving dangerously low blood pressure, abnormal heart rhythms, and kidney failure, that sometimes results in death.
Cannabis and Heart Risks in Summary
Despite this seemingly bleak picture, cardiovascular events only represent 2% of all medical reports related to cannabis. Cannabis’ relationship with cardiovascular health remains unclear, and we’re left inferring its effects from the impacts of THC on its own or generalizing from the effects of activating CB1 or CB2 receptors in preclinical animal models.
Emerging evidence suggests that cannabis use increases risk for cardiovascular events, but these studies fail to control for THC levels consumed, the presence of additional and often counteracting cannabinoids (e.g., CBD), duration and frequency of use, and consumption method. Regardless of how you interpret the risk, just be sure stay away from synthetic cannabinoids like K2 and Spice—that junk can kill you.